Advertisement
Advertisement
March/April 2018
Sponsored by BioTrace Medical Inc.
Rethinking the Temporary Pacing Lead
The Tempo® Lead from BioTrace Medical Inc. delivers safe lead placement, secure pace capture, and postprocedure ambulation.
The need for safe, stable temporary pacing during balloon aortic valvuloplasty (BAV) as well as valve deployment and to manage conduction disturbances during and postprocedure has increased with the rapid adoption of transcatheter aortic valve replacement (TAVR). In the past, surgical aortic valve replacement relied on surgically placed temporary epicardial pacing leads to support perioperative conduction disturbances. With the shift to TAVR, there has been a parallel move to transvenous temporary pacing; however, fundamental complications remain.
LIMITATIONS OF STANDARD TEMPORARY PACING LEADS
Standard temporary pacing leads are used to support patients with transient bradyarrhythmias. Recent clinical studies of patients undergoing TAVR have confirmed complications related to standard temporary transvenous pacing, which contribute to postprocedural mortality and morbidity.1-4 Specifically, pacing leads are associated with serious complications including cardiac perforation (up to 4%) and dislodgment (10%–37%) with loss of pace capture.5-10 In addition to posing intraprocedural risk, these design limitations may substantially impact postprocedural use, confine patients to bed rest, and contribute to costly length of stay (LOS) in the intensive care unit. In the search for pacing stability and ambulation capabilities, some institutions have resorted to using more expensive permanent pacing leads for temporary implantation.
Despite the limitations of current pacing leads, improvement of temporary pacing has been minimal for decades. Standard pacing leads have two electrodes with one rigid metal electrode at the distal tip. The rigid, sharp distal tip predisposes the leads to myocardial perforation. The leads are also unstable due to the lack of a myocardial fixation modality. Therefore, there is an unmet need for a secure and stable temporary pacing lead technology for TAVR and other applications that improves the safety and efficacy of current leads, minimizes repositioning, reduces complications, and enables earlier ambulation and quicker patient recovery.
THE TEMPO LEAD: SIGNIFICANT ADVANCEMENT IN TEMPORARY PACING
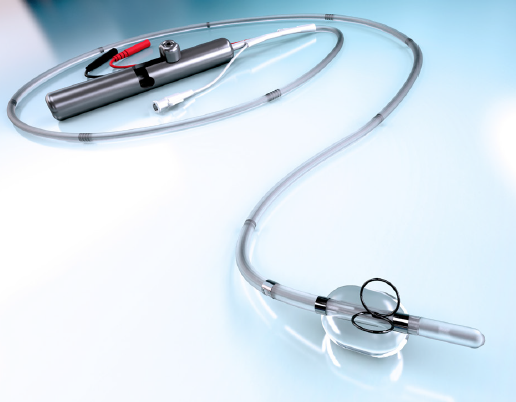
Figure 1. The Tempo Lead features active fixation, bipolar electrodes, and a soft tip to reduce the risk of right ventricle perforation and to ensure stable pace capture.
The Tempo Lead (Figure 1) was created to resolve the limitations of current temporary pacing leads. It can be used in conjunction with TAVR or any procedure requiring temporary pacing, such as alcohol septal ablation, BAV, or electrophysiology studies. Developed for secure and stable pacing, the Tempo Lead is designed to mitigate the previously mentioned complications and enable earlier patient ambulation. It is the only active fixation temporary lead that is commercially available in the United States and has a cleared indication by the US Food and Drug Administration for use up to 7 days.
“The Tempo Lead is the first major improvement in pacing lead fixation entering clinical use in more than 30 years,” said Tamim Nazif, MD, Director of Clinical Services, Structural Heart & Valve Center at New York-Presbyterian/Columbia University Medical Center in New York, New York. “Advantages of this unique fixation process include minimizing perforation risk, achieving a stable pace capture threshold (PCT), and minimizing risk of capture loss and embolization.”
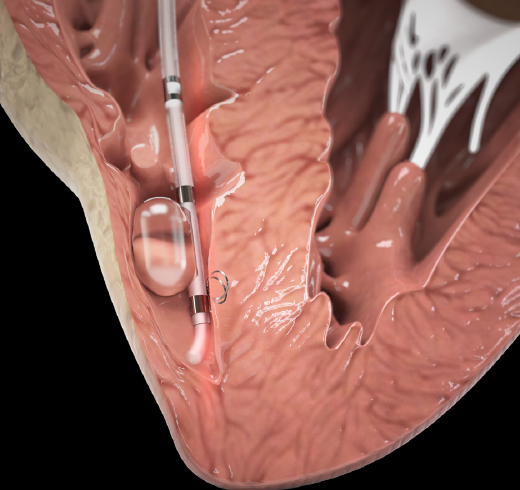
Figure 2. The Tempo Lead’s active fixation is accomplished via retractable stabilizer loops deployed into the myocardium. An elastomeric balloon inflates to aid passage through the venous vasculature and into the right ventricle and provides apposition of the loops to the myocardium.
In place of a rigid tip, the Tempo Lead has a soft distal tip to minimize the risk of right ventricle (RV) perforation or injury. Small, retractable wire loop stabilizers provide atraumatic myocardial fixation (Figure 2). The lead is most commonly inserted from the femoral or jugular vein. An elastomeric balloon that is mounted asymmetrically on the lead body between the electrodes inflates to aid passage of the lead into the RV and enhances wall apposition of the stabilizing loops. A small handle is used to deploy the stabilizers with an easy, one-handed maneuver. Once the stabilizers are in place, the balloon is deflated and the lead is left securely in place. The 6-F lead is shapeable, easily visualized, and compatible with all available external pulse generators.
“If we have a temporary pacing lead that is safer, maintains capture, and reduces perforations, then we could change our clinical care pathways by ambulating patients sooner and waiting longer before deciding to implant a permanent pacemaker,” said Susheel K. Kodali, MD, Director of the Structural Heart & Valve Center at New York-Presbyterian/Columbia University Medical Center. “The Tempo Lead’s dependable and stable pace capture provides physicians a better postprocedure temporary pacing solution with the potential for quicker ambulation and reduced cost.”
INTRAPROCEDURAL SAFETY AND RELIABLE Pace Capture
The safety and technical feasibility of the Tempo Lead was first demonstrated in a prospective, single-arm, nonrandomized study. The 25 patients (60% women; mean age, 64 ± 19 years) underwent 13 TAVR procedures (seven with Sapien 3™, Edwards Lifesciences; four with CoreValve™, Medtronic; and two with LOTUS, Boston Scientific Corporation), 11 electrophysiology procedures, and one BAV at two New Zealand centers.11
The Tempo Lead was successfully positioned in 23 (92%) cases; two patients had unsuitable anatomy. The safety endpoint of freedom from pericardial effusion requiring intervention and/or echocardiographic evidence of tamponade was met in all patients, with no device-related adverse events. No patient experienced sustained ventricular arrhythmia or lead dislodgment. The average final procedural PCT was 0.7 ± 0.5 milliamperes (mA). Rapid pacing was successful in all cases with no loss of capture. When surveyed, operators reported that the lead was easy to position and use, the stabilizers were easily deployed, and the soft tip contributed to the safe use of the lead.11,12
These results were further demonstrated by a multicenter, investigator-initiated, United States retrospective study of the safety and efficacy of the Tempo Lead (Table 1). Data was collected from five centers for 224 consecutive patients (35% women; mean age, 77 ± 10.5 years) who underwent use of the Tempo Lead for temporary pacing (62% TAVR with CoreValve or Evolute™, 33% TAVR with Sapien 3, 4% alcohol septal ablation, and 1% other). The study evaluated safety (including perforation, new pericardial effusion, and sustained device-related arrhythmias) and efficacy, defined as clinically acceptable pacing thresholds with stable pace capture over the duration of temporary implant.13
The Tempo Lead was successfully positioned and affixed in the right ventricle in 219 (98%) cases in the retrospective study. A total of 93 (42%) cases were accessed femorally and 131 (58%) cases used internal jugular venous access. In five cases, the Tempo Lead could not be placed due to unsuitable anatomy. There were no reported device-related adverse events, including no perforations, pericardial effusions, or sustained device-related arrhythmias. Procedural mean PCT was 0.7 ± 0.6 mA (n = 213). This study of the initial United States experience demonstrates that the Tempo Lead is safe and effective for temporary cardiac pacing and provides stable periprocedural pacing support.13
POSTPROCEDURE SAFETY, STABILITY, AND AMBULATION
The safety, stability, and early ambulation benefits of the Tempo Lead’s active fixation for secure and stable cardiac pacing were demonstrated in both the first-in-human study and the retrospective analysis discussed earlier. In the first-in-human study, the Tempo Lead remained in five patients between 9 hours and 5 days. The patient with the 5-day duration was pacing dependent and ambulated with stable PCTs and a final PCT of 1.5 mA.11
In the retrospective multicenter analysis, the Tempo Lead was used postprocedure in 159 (71%) patients, had a mean implant time of 42 hours, and final PCT was 0.8 ± 1 mA (n = 85). In addition, 137 (86%) patients ambulated postprocedure with the Tempo Lead in place for a mean of 45 hours, with average stable PCTs of 0.8 ± 1.1 mA (n = 73).13 These clinical data demonstrate that the Tempo Lead provides stable postprocedural pacing support and facilitates postprocedure ambulation.
“Traditional temporary pacing leads frequently cause complications, which result in additional time for the physician and longer hospital stays for the patient,” said Stanley J. Chetcuti, MD, Associate Professor of Internal Medicine and Director of the Cardiac Catheterization Laboratory at University of Michigan in Ann Arbor, Michigan. “With the Tempo Lead, patients are safely ambulating during observation, which allows for early discharge, reduced hospital costs, and more blissful sleep for the on-call team.”14
CASE STUDY: TAVR LENGTH OF STAY REDUCTION
The Tempo Lead’s novel design facilitates secure and stable cardiac pacing and enables patients to ambulate as soon as “day 0” postprocedure, resulting in benefits associated with a reduced hospital LOS.15 Many hospitals are moving to bundled payment initiatives as a result of the Centers for Medicare & Medicaid Services (CMS) bundled payment initiative and the Affordable Care Act. In the case of TAVR, the levers for success under CMS are decreased skilled nursing facility (SNF) utilization and reduction in hospital readmission rates.
“Our hospital recognized that the postacute care setting provides a great opportunity to initiate the shift from volume- to value-based care and concurrently achieve better patient care, better outcomes, and lower costs,” said Carlos Sanchez, MD, FACC, FSCAI, with OhioHealth Riverside Methodist Hospital in Columbus, Ohio.
Riverside Methodist Hospital created a risk-stratifying tool to identify patients with modifiable clinical risk and then developed a systematic approach to reduce the risk. In response to CMS levers, goals were established to reach a 30-day TAVR readmission rate of < 10% and achieve SNF utilization of < 0.80 observed-to-expected ratio.
“The goals of reducing readmission rates and decreasing SNF utilization adversely impacted a third goal of reducing hospital LOS,” summarized Steven J. Yakubov, MD, FACC, FSCAI, with OhioHealth Riverside Methodist Hospital.
During implementation of the new CMS-driven model, the hospital significantly reduced readmissions to 4% and exceeded its goal of reduced SNF utilization, moving from a baseline of 0.94 to 0.5 observed-to-expected ratio. However, these reductions resulted in an increase in LOS from 2.5 to 3.1 days. Patients were kept in the hospital longer for observation, physical therapy, and/or occupational therapy.15
“This was not the outcome Riverside Methodist was trying to achieve, especially as TAVR evolves to a minimalist approach and administrators want to discharge those patients sooner,“ Dr. Yakubov explained.
In response, the cardiac team at Riverside Methodist was tasked with creating a new initiative that would decrease the hospital LOS. They recognized that physical therapy would need to begin as early as postprocedure day 0 to achieve this goal. However, a dated hospital policy prevented getting patients with any type of temporary pacemaker in place out of bed. Enter the Tempo Lead. The team devised an internal comparison to demonstrate that the Tempo Lead enabled safe ambulation of patients postprocedure.
A total of 27 patients (26% women; average age, 78 years) were evaluated using the Tempo Lead during the patient’s TAVR procedure and remained affixed postprocedure to manage conduction disturbances (Table 2). With the active fixation, the team was comfortable getting the patients out of bed and starting physical therapy on postprocedure day 0. The Tempo Lead’s success rate for all 27 patients was 100%.15
“The resulting policy change had the desired impact. The Tempo Lead allowed early ambulation and early physical therapy for post-TAVR patients, especially those at high risk,” said Dr. Yakubov. “The 27-patient comparison achieved a reduction in LOS from 3.1 to 1.7 days, while maintaining the 30-day hospital readmission rate at 4%.”15
CONCLUSION
With its novel active fixation mechanism designed to enhance pacing stability and a soft tip to mitigate perforation, the Tempo Lead demonstrates safety and efficacy for temporary cardiac pacing, provides stable peri- and postprocedural support, and facilitates postprocedure ambulation.13 The Tempo Lead’s clinical and economic benefits are being validated on a large scale, with more than 1,000 placements performed to date without a reported adverse event.
“Innovation has finally come to temporary pacing,” said Brian K. Whisenant, MD, Medical Director, Heart Valve and Structural Heart Disease for the Intermountain Heart Institute in Salt Lake City, Utah. “The Tempo Lead is poised to play a pivotal role in improving patient outcomes, reducing intensive care unit LOS, and lowering hospital cost.”
1. Piazza N, Onuma Y, Jesserun E, et al. Early and persistent intraventricular conduction abnormalities and requirements for pacemaking after percutaneous replacement of the aortic valve. J Am Coll Cardiol Interv. 2008;1:310-316.
2. Grube E, Buellesfeld L, Mueller R, et al. Progress and current status of percutaneous aortic valve replacement: results of three device generations of the CoreValve Revalving system. Circ Cardiovasc Interv. 2008;1:167-175.
3. Cribier A, Eltchaninoff H, Tron C, et al. Treatment of calcific aortic stenosis with the percutaneous heart valve: mid-term follow-up from the initial feasibility studies: the French experience. J Am Coll Cardiol. 2006;47:1214-1223.
4. Bosmans JM, Kefer J, De Bruyne B, et al. Procedural, 30-day and one year outcome following CoreValve or Edwards transcatheter aortic valve implantation: results of the Belgian national registry. Interact Cardiovasc Thorac Surg. 2011;12:762-767.
5. Lumio FJ, Rios JC. Temporary transvenous pacemaker therapy. Analysis of complications. Chest. 1973;64:604-608.
6. Gammage MD. Temporary cardiac pacing. Heart. 2000;83:715-720.
7. Murphy JJ. Current practice and complications of temporary transvenous cardiac pacing. BMJ. 1996;312:1134-1147.
8. López Ayerbe J, Villuendas Sabaté R, García C, et al. Temporary pacemakers: current use and complications. Rev Esp Cardiol. 2004;57:1045-1052.
9. Austin JL, Preis LK, Crampton RS, et al. Analysis of pacemaker malfunction and complications of temporary pacing in the coronary care unit. Am J Cardiol. 1982;49:301-306.
10. Betts TR. Regional survey of temporary transvenous pacing procedures and complications. Postgrad Med J. 2003;79:463-466.
11. Webster M, Pasupati S, Lever N, Stiles M. TCT-840 first-in-human experience with a novel active fixation temporary pacing lead: safety and efficacy of the Tempo Lead. JACC. 2016;68:B339-B340.
12. Webster M, Pasupati S, Lever N, Stiles M. Safety and feasibility of a novel active fixation temporary pacing lead [published online February 15, 2018]. J Invasive Cardiol.
13. Nazif T, Sanchez C, Whisenant B, et al. Session 1243-225 interventional cardiology: aortic, mitral and structural heart disease – analysis of the initial United States experience with the BioTrace Tempo temporary pacing lead in transcatheter aortic valve replacement (TAVR) and other cardiac procedures. Presented at: American College of Cardiology (ACC).18; March 10–12, 2018; Orlando, Florida.
14. Chetcuti SJ. Post-TAVR Tempo Lead placement and patient ambulation. Presented: at: 2017 Transcatheter Cardiovascular Therapeutics Congress; October 29–November 2, 2017; Denver, Colorado.
15. Yakubov S. How to manage pacemakers with TAVR, temporary and permanent indications. Presented at: 2017 Transcatheter Cardiovascular Therapeutics Congress (virtual session); October 29–November 2, 2017; Denver, Colorado.

3925 Bohannon Drive, Suite 200
Menlo Park, CA 94070
www.biotracemedical.com
info@biotracemedical.com
P: 650.779.4999 | F: 650.779.4746
Advertisement
Advertisement


