Advertisement
Advertisement
September/October 2020
Tips and Tricks to Performing the Crossover Technique
A detailed description of how to perform the crossover technique, anatomic considerations, and potential complications.
By Tarek A. Hammad, MD, and Mehdi H. Shishehbor, DO, MPH, PhD
Although the common femoral artery (CFA) still dominates as the entry site for percutaneous coronary interventions performed in the United States, femoral access complications continue to be the most common procedural ramification. Some of these can be limb- or even life-threatening, especially if not recognized and managed in a timely manner. Every interventionalist should have the skill set required to readily manage such adversities as they arise. This is very relevant to today’s practice, where the number of procedures requiring large-bore access, such as with percutaneous mechanical circulatory support devices and structural interventions, are on the rise and the transfemoral approach is the preferred access modality. Notably, many interventionalists are not familiar with the “crossover” technique and do not realize that it can bail them out in most cases. This article describes the crossover technique in detail, which is the mainstay for the execution of any subsequent intervention.
HOW I DO IT
Using two-dimensional ultrasound and fluoroscopic guidance, the CFA is cannulated over the femoral head, 1 to 2 cm above the femoral bifurcation and below the origin of the inferior epigastric artery, using the modified Seldinger technique. In our practice, we always use a micropuncture vascular access kit; once a blood return is observed via the 21-gauge needle, a 0.014-inch wire is advanced with caution through the needle. A quick fluoroscopic image is obtained to confirm the location of needle entry and the course of the microwire. Next, the needle is removed while maintaining wire position, and a 4-F micropuncture sheath is advanced over the 0.014-inch wire. The latter is exchanged to a 0.035-inch Wholey wire (Medtronic), which is advanced under fluoroscopic guidance into the thoracic descending aorta. Subsequently, the micropuncture sheath is replaced by a short 5-F femoral sheath. A 5-F diagnostic internal mammary (IM) catheter is advanced via the femoral sheath and over the Wholey wire until its tip is several centimeters above the abdominal aortic bifurcation. The Wholey wire is pulled back proximal to the IM catheter tip, and the IM catheter is gently torqued and slowly withdrawn until its tip engages the ostium of the contralateral common iliac artery. This can be verified by advancing the Wholey wire beyond the tip of the IM catheter and observing its course before removing it outside the body.
After confirming normal arterial waveform and pressure, digital subtraction angiography (DSA) of the contralateral iliofemoral system is performed using a large field of view (typically 42 cm) with the image intensifier angulated at 30° contralaterally (right anterior oblique for the left iliofemoral system and left anterior oblique for the right iliofemoral system). It is vital to instruct the patient to hold his/her breath and stay still during image acquisition. We also advise for a long run of the DSA, especially when suspecting vessel occlusion, to help identify the level of the reconstitution and the course of the vessels of interest as they fill in a retrograde fashion via collaterals. If an intervention is deemed necessary, reintroduce the Wholey wire through the IM catheter and advance it as far as possible into the contralateral superficial femoral artery (SFA) or the profunda artery. Then, remove the IM catheter, and replace the 5-F, short femoral sheath with a 6-F, 55-cm Flexor Ansel sheath (Cook Medical) over the Wholey wire and park its tip proximal to the targeted segment.1
The next step depends on the underlying problem; there are typically three common scenarios:
1. If there is an acute closure of the CFA such as in the case of Perclose ProGlide (Abbott) suture capturing the posterior wall of the vessel, we usually attempt to cross the occlusion with a 0.035-inch, stiff angled Glidewire (Terumo Interventional Systems; a 0.018-inch Glidewire Gold is an alternative) with the support of a 0.035-inch NaviCross catheter (Terumo Interventional Systems). Once the occlusion is traversed, the NaviCross support catheter is advanced past the occlusion and the wire is exchanged back to the safe supportive Wholey wire. The suture knot can be broken by inflating a short peripheral balloon (usually 6 X 40 mm) at low pressure over the Wholey wire. We repeat DSA of the area of interest to ensure restoration of normal blood flow and the absence of other complications including bleeding, dissection, or thrombosis.
2. If the underlying problem is bleeding secondary to failure to close the access site, then the same aforementioned peripheral balloon can be advanced over a Wholey wire and inflated at nominal pressure for 15 to 20 minutes while watching for signs and symptoms of limb ischemia. Once the balloon is inflated, we typically repeat the DSA to ensure there is no contrast extravasation. In some cases, a Viabahn covered stent (Gore & Associates) may be necessary.
3. When performing a final groin angiogram without a wire in the abdominal aorta to direct the sheath tip away from the external iliac artery wall and maintain access, iatrogenic hydraulic retrograde dissection may occur. After crossing up and over from the contralateral groin and engaging the ostium of the ipsilateral common iliac artery with an IM catheter, DSA is performed to assess the blood flow. If the blood flow is compromised, then the true lumen is crossed using a Wholey wire, and an appropriately sized balloon is inflated with or without a stent to tack the dissection.
A list of required materials for the crossover technique is shown in the sidebar.
MATERIALS REQUIRED FOR THE CROSSOVER TECHNIQUE
- Sheaths: 4-F micropuncture, 5-F regular femoral sheath, and 6-F, 55-cm Flexor Ansel sheath (alternatives: any 6-F, 40-60-cm sheath such as a Flexor Raabe [Cook Medical] and Pinnacle Destination [Terumo Interventional Systems]); keep in mind that the planned intervention will dictate the final sheath size, but a 6- to 7-F sheath is usually adequate
- Catheters: 5-F IM diagnostic catheter (alternatives: SOS Omni, AngioDynamics; Simmons, Merit Medical Systems, Inc.) and 0.035-inch NaviCross catheter, which can be used for exchanging wires or providing support
- Wires: 0.035-inch Wholey wire (or Hi-Torque Versacore wire [Abbott]), 0.035-inch stiff angled Glidewire, and 0.018-inch Glidewire Gold
- Balloon: 6- X 40-mm peripheral balloon, which may vary in size depending on the size of the CFA
- Covered stent: 6- X 40-mm Viabahn stent
It is helpful to put together a crossover kit that contains the above equipment and make it available in every interventional catheterization laboratory.
ANATOMY
Certain anatomic features may make crossover very challenging. A Judkins right catheter can help the wire steer iliac tortuosity. The operator may also choose to exchange to a 25-cm sheath first to bypass severe tortuosity of the iliac artery on the access side. Advancing a stiff angled Glidewire with caution can help navigate a severely tortuous iliac artery on either side, but the operator must be sure to exchange this with a safe, supportive 0.035-inch wire (such as a Wholey wire) before proceeding with sheath exchange and intervention.
Difficulty in tracking the sheath over the wire is commonly encountered. The first step is usually to use a stiffer wire and advance it as far as it can reach. If it’s still a struggle, then apply constant pressure to advance the sheath while pulling the wire (the “paradoxical move” technique). If this does not work, then perform the “Dottering” technique by moving the wire gently backward and forward while applying constant forward pressure on the sheath to help decrease wire wall bias and center the sheath for easier advancement. If still unsuccessful, free the dilator from the sheath and walk the sheath over the dilator in small steps with a great amount of care to avoid vessel wall injury. Then, follow the sheath with the dilator and repeat walking the sheath over the dilator as needed. In extreme cases, the “balloon-assisted tracking” technique can be used. Inflate a balloon in the SFA or the profunda artery at a nominal pressure to stabilize the wire and create a strong rail over which the sheath can be advanced (Figure 1). An acute angulation of the abdominal aortic bifurcation can make wire and/or sheath advancement unfeasible despite all the previously mentioned maneuvers. In such a situation, special catheters such as a Simmons or SOS Omni can overcome this problem; however, these catheters need to be shaped in the aortic arch, and therefore heparinization is advised. The presence of kissing iliac stents makes crossover impossible, so radial access needs to be considered (Figure 2).2

Figure 1. Balloon-assisted tracking technique. In this patient, there was great difficulty advancing the sheath into the contralateral femoral system; therefore, a 5- X 40-mm peripheral balloon was inflated in the contralateral SFA at low pressure to stabilize the wire and create strong rail while pulling on the other end of the wire. This technique allowed us to advance the 6-F, 55-cm sheath easily into the contralateral CFA.
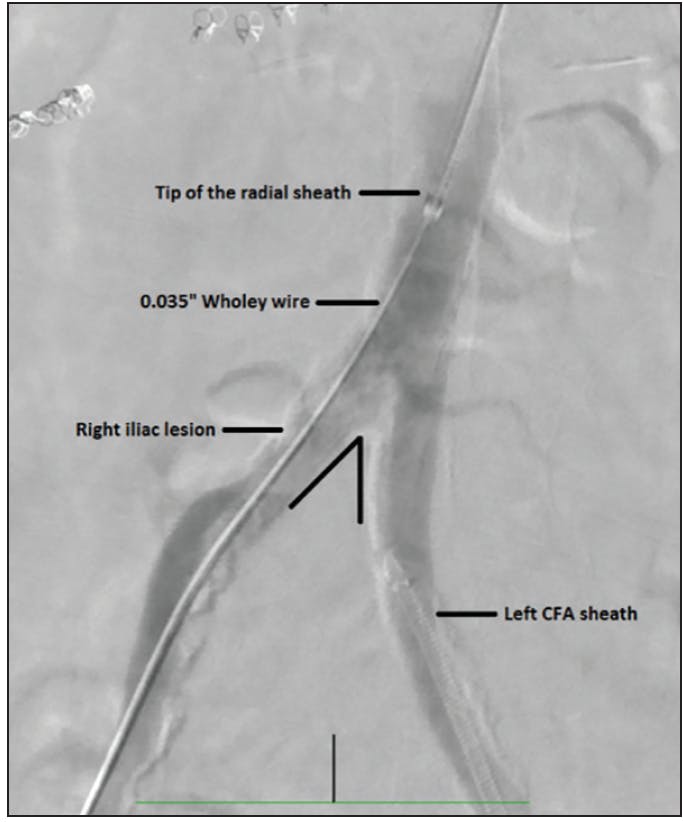
Figure 2. Radial access for acute angulation of the abdominal aortic bifurcation. Note the acute angulation of the abdominal aortic bifurcation. An SOS or Simmons catheter may have performed well in crossing over. However, in this patient, we choose to proceed with radial access because there was also a significant ostioproximal right iliac lesion that needed treatment. After achieving right radial access, we crossed into the right iliac artery using an 0.035-inch wire with the help of an IM catheter. Then, a long 6-F, 119-cm R2P radial sheath (Terumo Interventional Systems) was introduced into the distal abdominal aorta over the Wholey wire.
COMPLICATIONS
Complications are rare in skilled hands using careful technique (1%-2%); however, some can be lethal. The most serious complication is perforation of the iliac artery with retroperitoneal hematoma. Immediate balloon tamponade with reversal of anticoagulation might be sufficient, but a covered stent should be always available. Other complications include dissection or thrombosis with resultant acute limb ischemia, hematoma, other types of bleeding, arteriovenous fistula, and pseudoaneurysm.
Remember that the crossover technique is often performed because the patient already had a complication. The initial problem may be access site closure with subsequent thrombosis and limb ischemia, while the subsequent complication might be iliac perforation with retroperitoneal bleed. The management of both can be extremely challenging; thus, we would like to emphasize that an experienced interventionalist with endovascular expertise must be notified before proceeding with crossover, so he/she can be immediately available if needed. It is also crucial to practice these techniques in a few routine elective cases, so the operator does not perform his/her first crossover in an emergent situation.
SUMMARY
The crossover technique enables coronary and structural interventionalists to treat most femoral access site complications before it is too late and in a minimally invasive way. Therefore, every interventionalist is highly encouraged to learn and master this technique to save his/her patient when needed. In addition, we advocate that every catheterization laboratory must have a designated kit for performing crossover.
1. Casserly IP, Sachar R, Yadav JS, editors. Practical Peripheral Vascular Intervention. 2nd ed. LWW; 2011.
2. Grenon SM, Reilly LM, Ramaiah VG. Technical endovascular highlights for crossing the difficult aortic bifurcation. J Vasc Surg. 2011;54:893-896. doi: 10.1016/j.jvs.2011.03.268
Advertisement
Advertisement

