Advertisement
Advertisement
July/August 2016
MitraClip in the United States
Commercial use and COAPT trial updates.
By Mike Saji, MD, and D. Scott Lim, MD
Mitral regurgitation (MR) is the most prevalent valvular heart disease in the United States.1 Transcatheter mitral valve repair (TMVR) using the MitraClip device (Abbott Vascular) is one of the few approved transcatheter options for patients with severe MR and is based on the surgical method developed by Alfieri et al.2 To date, more than 30,000 procedures have been performed globally.3,4 On October 25, 2013, the MitraClip device was approved by the US Food and Drug Administration (FDA) for commercial use in the United States in patients with degenerative MR who are at prohibitive risk (Figure 1). This approval was based on data from the EVEREST II trial and European experience.3-5 However, the FDA has not approved the use of MitraClip for patients with functional MR (Figure 2) in the United States, despite an approximate usage rate of 80% in these patients in Europe. Instead, the FDA has approved the COAPT trial (NCT01626079), in which patients with functional MR receive optimal medical therapy and are then randomized to either continuation of medical therapy or medical therapy and the MitraClip device.
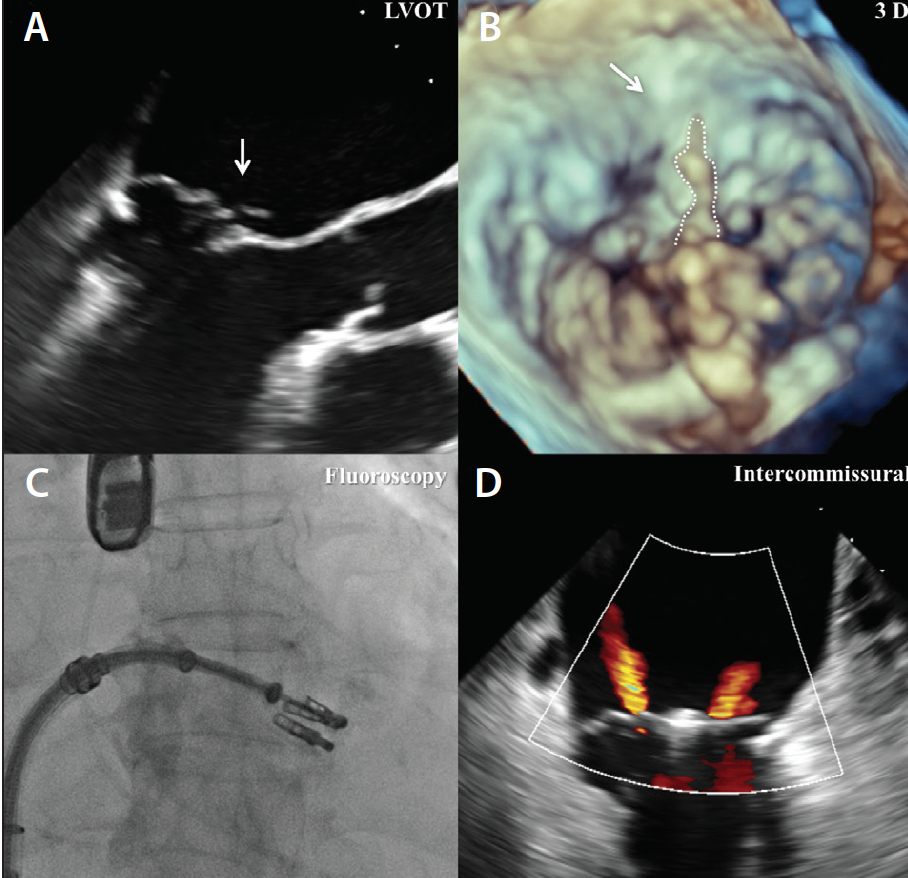
Figure 1. Example of degenerative MR due to flail leaflet; primary pathology was clipped by the first MitraClip; however, there was significant residual jet on the lateral side of the first clip. The second MitraClip was placed lateral to the first MitraClip. Final MR was mild on transesophageal echocardiography. Left ventricular outflow tract (LVOT) view showing P2 mitral valve scallop flail with torn chord (A). Threedimensional view showing P2 mitral valve scallop flail with torn chord (B). Additional clip being placed laterally after first clip placed on primary pathology (C). Intercommissural view showing mild MR with two MitraClips (D).
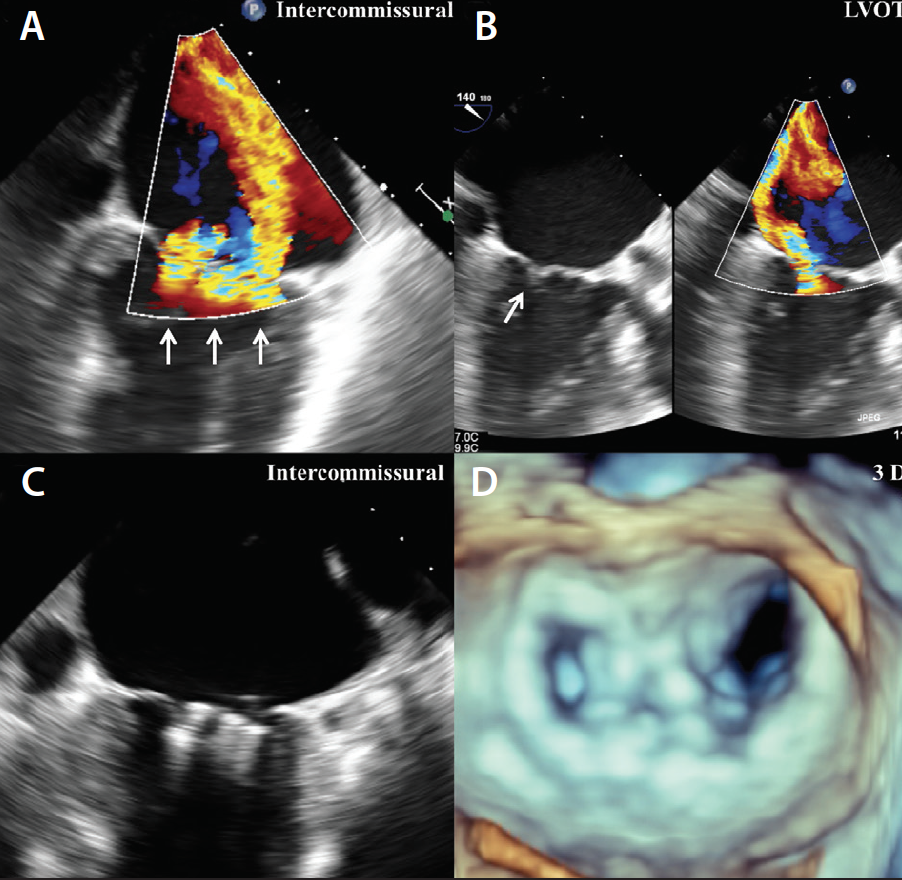
Figure 2. Example of functional MR; ischemic cardiomyopathy on the posterior wall resulted in severe MR due to restricted posterior leaflet. Intercommissural view showing wide regurgitant jet (A). LVOT view showing restricted posterior leaflet with posterior directed jet view (B). Intercommissural view showing three clips placed in A2-P2 mitral valve leaflet (C). Three-dimensional view showing a double orifice created by three MitraClips (D).
COMMERCIAL USE OF MITRACLIP
After United States approval of the MitraClip device for commercial use in prohibitive-risk patients with degenerative MR, there have been recommendations for use based on multisociety guidelines.6 Despite a poor correlation between the EuroSCORE and Society of Thoracic Surgeons (STS) score, patients are usually classified as high risk for open heart surgery when the scores are > 20% and 8%, respectively, the heart team (consisting of a cardiologist, surgeon, and anesthesiologist) observes that patients have significant comorbidities (eg, hostile chest, porcelain aorta, severe liver disease, severe pulmonary hypertension, internal mammary artery crossing the midline), or frailty is not reflected in those scores.7 Recent publication of the 30-day results from the STS/American College of Cardiology TVT registry provided support for the utility of the MitraClip therapy in patients with degenerative MR.8 During the period from November 2013 to August 2014, 564 patients had their data entered into the registry. The average age was 83 years, and 86% were New York Heart Association functional class ≥ III, with a median STS score of 10% for surgical mitral valve replacement. The majority of the patients were elderly and had a high prevalence of significant morbidities, including frailty. Acute procedural success, defined as a composite of postimplantation MR ≤ grade 2 without conversion to open cardiac surgery and absence of in-hospital mortality, was 93%. In-hospital mortality and 30-day mortality were 2.3% and 5.8%, respectively. Procedural complications, mainly consisting of major bleeding, occurred in 8%, and device-related complications were low (1.3%). Length of hospital stay was short (median, 3 days), with 84% of patients discharged directly to home. Given that this initial commercial experience included new MitraClip operators, these results are favorable compared with the results demonstrated in preapproval research studies, as well as those reported in other national and multinational registries.3,4,9
In a multivariate logistic regression model, successful MR reduction was associated with smaller end-diastolic dimension, lower preprocedural MR severity, pathology location (A2–P2), and higher case volume per institution. Notably, TMVR using the MitraClip device was available at 61 sites in the United States, meaning the results obtained from the multivariate model should be interpreted with caution given the low volume per site and high concentrations of patients at a few centers (median number of cases per institution, 6). Additionally, echocardiographic variables are site reported and not assessed by a core laboratory. For these reasons, data adjudication was limited. Nonetheless, postmarket approval registries provide valuable information on MitraClip use in the commercial setting and support the continued role of TMVR using the MitraClip by the heart team in the treatment of degenerative MR in patients who are at prohibitive risk.
More recently, United States commercial use of MitraClip and 1-year data from the TVT registry were updated (unpublished data on file at Abbott Vascular), which includes a total of 4,019 patients from 212 sites in the United States. When compared with the 61 sites involved in the 30-day outcomes and the 42 sites involved in previous research trials, it becomes evident that MitraClip case volumes have been dramatically growing (2,503 procedures performed in 2015). In these data, the average age was 79 years, and 87% were New York Heart Association functional class ≥ III. The majority of the patients had significant morbidities, with a high incidence of frailty and similar 30-day outcomes. The 1-year mortality was 2.2%, and 92% had MR ≤ 2 after the procedure, with a low rate of procedural complications, including a major vascular complication rate of 0.3% (significantly decreased compared with previously reported vascular complications). The length of hospital stay was shorter (mean, 5 days; median, 2 days), with 87% of patients discharged directly to home. Fewer than 1% of the patients required reintervention.
THE COAPT TRIAL
The COAPT trial is the first randomized controlled trial to compare the nonsurgical standard-of-care treatment to a transcatheter intervention to decrease MR. This trial is important as a landmark trial to further study the MitraClip device in symptomatic functional MR patients with heart failure (HF). It will provide a clinically and economically important base of information to support reimbursement and evidence to enable the development of treatment guidelines in patients with functional MR. The trial is designed to confirm the safety and effectiveness of the MitraClip system for the treatment of moderate-to-severe or severe functional MR with 1:1 randomization (MitraClip arm and standard-of-care arm). Follow-up will continue for up to 60 months after the TMVR procedure in symptomatic HF patients who are treated per guideline-directed standard of care and have been designated by the site’s local heart team as not appropriate for mitral valve surgery.
The primary endpoints are recurrent HF hospitalizations through 24 months (analyzed when last patient completes 12-month follow-up) and a composite of single-leaflet device attachment, device embolization, endocarditis requiring surgery, core lab-confirmed mitral stenosis requiring surgery, left ventricular assist device implantation, heart transplantation, and any device-related complication requiring nonelective cardiovascular surgery at 12 months.
The secondary endpoints are MR severity at 12 months, change in 6-minute walk test at 12 months, change in quality-of-life score (KCCQ) at 12 months, change in left ventricular end-diastolic volume, reduction to New York Heart Association functional class I/II at 12 months, hierarchical composite of death and recurrent HF hospitalization, all-cause recurrent hospitalizations (analyzed when last patient completes 12-month follow-up), and a composite of all-cause death, stroke, myocardial infarction, nonelective cardiovascular surgery for device-related complications in the device group at 30 days, and all-cause death at 12 months.
Key inclusion criteria for the COAPT trial include symptomatic functional (either ischemic or nonischemic) MR ≥ 3+; at least one HF admission in the 12 months prior to enrollment and/or brain natriuretic peptide (BNP) ≥ 300 pg/mL or NT-proBNP ≥ 1,500 pg/mL; adequate treatment with revascularization, cardiac resynchronization therapy, and/or optimized medical therapy; and noncommissural primary jet. In addition, surgery will not be offered as a treatment option, and medical therapy is the intended treatment for the patients.
Key exclusion criteria include inappropriate anatomy, mitral valve orifice area < 4 cm2, invasive procedures (eg, coronary bypass surgery, percutaneous coronary intervention, transcatheter aortic valve replacement, carotid surgery) within 30 days, cerebrovascular accident within 30 days, symptomatic severe carotid stenosis, severe right ventricular dysfunction, tricuspid or aortic disease requiring surgery, chronic obstructive pulmonary disease requiring continuous home oxygen therapy or chronic outpatient oral steroid use, and American College of Cardiology/American Heart Association stage D HF.
The trial was initially designed to enroll 430 patients, but was increased to now enroll 555 patients at up to 85 United States sites. The sample size has been increased to ensure that there is sufficient power to determine whether the MitraClip procedure does indeed reduce HF hospitalizations in functional MR. Recently (as of April 30, 2016), the number of randomized patients passed the 400 mark. In Europe, two similar randomized trials are being conducted—the RESHAPE HF (NCT01772108) and Mitra-FR (NCT01920698) trials.
FUTURE PERSPECTIVE
For patients with degenerative MR, MitraClip therapy is currently only approved for patients at prohibitive risk for mitral valve surgery. In the future, it is expected that there will be the option to combine repair techniques by adding catheter-delivered annuloplasty to the MitraClip procedure.10 An ongoing study in Europe, the HIRIDE (High and Intermediate Risk Degenerative Mitral Regurgitation Treatment) randomized trial (NCT02534155) will also provide further evidence and potentially expand the indication of MitraClip to patients at intermediate and high risk.
In patients with functional MR, major trials are still underway, and the role of this technology needs to be clarified. On the other hand, other techniques to treat functional MR are currently in the early phases of study and development, including the Tiara mitral valve system (Neovasc Inc.), Tendyne mitral valve system (Abbott Vascular, acquired from Tendyne Holdings, Inc.), CardiAQ mitral valve bioprosthesis (Edwards Lifesciences, acquired from CardiAQ Valve Technologies), and Twelve transcatheter mitral valve replacement system (Twelve, Inc.). Transcatheter mitral valve implantation raises some challenges such as its positioning, anchoring, thrombosis, left ventricular outflow tract obstruction, coronary circumflex artery impingement, and paravalvular mitral leak.
In the next 5 years, as has happened with open mitral surgery, transcatheter repair and replacement will likely have better-defined roles. Additional evidence should be accumulated by randomized studies comparing these new techniques, along with medical therapy of functional MR.11 Nonetheless, MitraClip is currently the most commonly utilized transcatheter therapy for severe MR with evidence of safety and effectiveness.
CONCLUSION
The initial commercial United States experience demonstrated the favorable procedural success rate that supports the effectiveness of the MitraClip in patients at prohibitive risk in a commercial setting. Looking ahead, COAPT will provide valuable information on patients with HF and secondary MR, and may also provide data for further expanding the indication of this device. No matter how the data look, it will be an important milestone in the field of transcatheter valve therapy.
1. Nkomo VT, Gardin JM, Skelton TN, et al. Burden of valvular heart diseases: a population-based study. Lancet. 2006;368:1005-1011.
2. Alfieri O, Maisano F, De Bonis M, et al. The double-orifice technique in mitral valve repair: a simple solution for complex problems. J Thorac Cardiovasc Surg. 2001;122:674-681.
3. Maisano F, Franzen O, Baldus S, et al. Percutaneous mitral valve interventions in the real world: early and 1-year results from the ACCESS-EU, a prospective, multicenter, nonrandomized post-approval study of the MitraClip therapy in Europe. J Am Coll Cardiol. 2013;62:1052-1061.
4. Puls M, Lubos E, Boekstegers P, et al. One-year outcomes and predictors of mortality after MitraClip therapy in contemporary clinical practice: results from the German transcatheter mitral valve interventions registry. Eur Heart J. 2016;37:703-712.
5. Lim DS, Reynolds MR, Feldman T, et al. Improved functional status and quality of life in prohibitive surgical risk patients with degenerative mitral regurgitation after transcatheter mitral valve repair. J Am Coll Cardiol. 2014;64:182-192.
6. Nishimura RA, Otto CM, Bonow RO, et al. 2014 AHA/ACC guideline for the management of patients with valvular heart disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines [published erratum appears in J Am Coll Cardiol. 2014;63:2489]. J Am Coll Cardiol. 2014;63:2438-2488.
7. Kappetein AP, Head SJ, Généreux P, et al. Updated standardized endpoint definitions for transcatheter aortic valve implantation: the Valve Academic Research Consortium-2 consensus document. J Am Coll Cardiol. 2012;60:1438-1454.
8. Sorajja P, Mack M, Vemulapalli S, et al. Initial experience with commercial transcatheter mitral valve repair in the United States. J Am Coll Cardiol. 2016;67:1129-1140.
9. Glower DD, Kar S, Trento A, et al. Percutaneous mitral valve repair for mitral regurgitation in high-risk patients: results of the EVEREST II study. J Am Coll Cardiol. 2014;64:172-181.
10. Maisano F, Taramasso M, Nickenig G, et al. Cardioband, a transcatheter surgical-like direct mitral valve annuloplasty system: early results of the feasibility trial. Eur Heart J. 2016;37:10:817-825.
11. Nishimura RA, Vahanian A, Eleid MF et al. Mitral valve disease—current management and future challenges. Lancet. 2016;387:1324-1334.
Mike Saji, MD
Department of Cardiology
Sakakibara Heart Institute
Tokyo, Japan
Disclosures: None.
D. Scott Lim, MD
Advanced Cardiac Valve Center
Department of Medicine, Division of
Cardiovascular Medicine
University of Virginia
Charlottesville, Virginia
(434) 243-1146; sl9pc@virginia.edu
Disclosures: Consultant for Abbott Vascular, Cephea Medical, Edwards Lifesciences, and St. Jude Medical; research funding from Abbott Vascular, Caisson Medical, Edwards Lifesciences, and St. Jude Medical.
Advertisement
Advertisement
