Advertisement
Advertisement
May/June 2018
Long-Term Efficacy of Percutaneous Mitral Commissurotomy for Mitral Stenosis
After successful PMC, what do the results show at 20 years?
By Alec Vahanian, MD, and Bernard Iung, MD
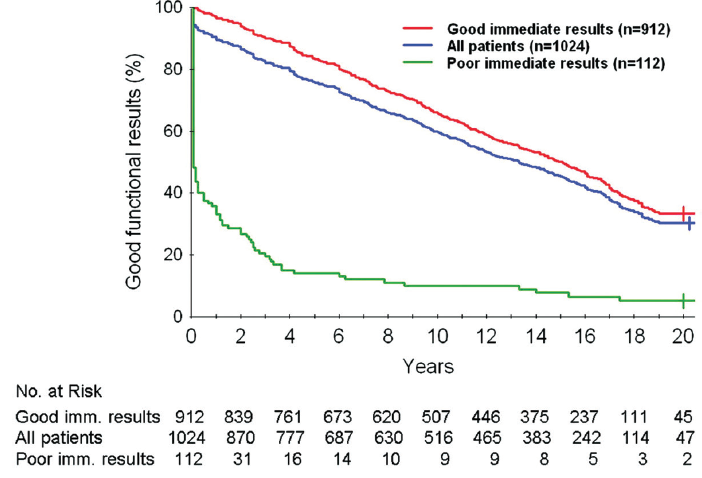
Figure 1. Twenty-year results of PMC survival without reintervention and NYHA class I or II. Good functional results after PMC in the entire population and according to immediate results. Good functional results are defined as survival considering cardiovascular-related deaths without mitral surgery or repeat PMC and in NYHA functional class I or II. Kaplan-Meier rates are presented with their standard errors. Reprinted from Bouleti C, Iung B, Laouénan C, et al. Late results of percutaneous mitral commissurotomy up to 20 years: development and validation of a risk score predicting late functional results from a series of 912 patients. Circulation. 2012;125:2119-2127.
Percutaneous mitral commissurotomy (PMC) is the treatment of choice for severe symptomatic mitral stenosis (MS) in the absence of contraindications.1,2 Results beyond 20 years are now available, which allow for the prediction of long-term results and, as a consequence, play an important role in patient selection.3-7 The overall clinical long-term results of PMC are good. In a large series from Europe, the 20-year rate of survival without intervention (either re-PMC or surgery) was 34.4% ± 2.1%, and 30.2% ± 2% of the patients were in New York Heart Association (NYHA) class I or II (Figure 1).4
Prediction of long-term results is multifactorial.3,4,8 It integrates clinical variables such as age, NYHA class before PMC, history of previous commissurotomy, severe tricuspid regurgitation, cardiomegaly, atrial fibrillation, high pulmonary vascular resistance, valve anatomy (as assessed by echocardiography scores), and the results of the procedure (ie, postprocedural valve area, mean mitral gradient after PMC). The various predictive factors of late functional results have been combined in a scoring system and are shown in Table 1.
LONG-TERM OUTCOMES PREDICTED BY IMMEDIATE RESULTS AFTER PMC
Poor Initial Outcomes
When the immediate results are unsatisfactory (valve area < 1.5 cm2 and/or mitral regurgitation > 2/4), midterm functional results are usually poor, and surgery, when feasible, is usually required shortly thereafter.4 If there is severe traumatic mitral regurgitation, early surgery is recommended, especially when it is associated with severe pulmonary hypertension. In the other cases, especially if the patient is symptomatic, surgery is indicated in the following weeks and close follow-up is required. Surgery should also be considered when mixed mitral disease or significant residual stenosis is present. The indications and the timing of surgery will depend on the patient’s symptoms and surgical risk. Close follow-up is needed and exercise evaluation may be helpful for determining the timing of surgery. Here, valve replacement is necessary in almost all cases because of the unfavorable valve anatomy responsible for the poor initial results.
Good Initial Outcomes
After successful PMC, the associated survival rates are excellent, the need for secondary surgery is infrequent, and functional improvement occurs in most cases. Twenty-year rates of cardiovascular survival without reintervention (repeat PMC or surgery) were estimated at 37.8% ± 2.3% and 33.3% ± 2.2% of the patients were in NYHA class I or II at last follow-up.4 When functional deterioration occurs, it is late and mainly related to restenosis.3,4,7-9
Restenosis
Restenosis following PMC has generally been defined by a loss of > 50% of the initial gain, with a valve area < 1.5 cm2. After successful PMC, the incidence of restenosis is usually low, between 2% and 40%, at time intervals ranging from 3 to 10 years. Reintervention is indicated when symptoms or pulmonary hypertension occur. Re-PMC can be considered in selected patients: (1) who have had an initially successful PMC, (2) if restenosis occurs after several years, (3) if there are favorable characteristics for PMC, and (4) if the predominant mechanism of restenosis is commissural refusion.10 In the other cases, including those with unicommissural refusion where the other commissure remains open, surgery should be considered.11 In patients with restenosis who remain asymptomatic, follow-up visits should be more frequent. Finally, PMC may have a palliative role in patients who present with suboptimal valve anatomy for PMC, but who are also not surgical candidates.
Follow-Up Protocols
Follow-up studies using sequential echocardiography have shown that the degree of mitral regurgitation on the whole remains stable, or slightly decreased, during follow-up.12 Atrial septal defects will close later in most cases. The persistence of shunts is related to their magnitude or to unsatisfactory relief of MS. Successful PMC also reduces embolic risk.13 There is no direct evidence that PMC reduces the incidence of atrial fibrillation.14
CONCLUSION
The long-term results of PMC are satisfactory up to 20 years after a successful PMC procedure. Follow-up after PMC mainly relies on a comprehensive examination early after PMC and a timely and appropriate indication for subsequent reintervention.
1. Nishimura RA, Otto CM, Bonow RO, et al. 2017 AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on clinical practice guidelines. J Am Coll Cardiol. 2017;70:252-289.
2. Baumgartner H, Falk V, Bax JJ, et al. 2017 ESC/EACTS Guidelines for the management of valvular heart disease. Eur Heart J. 2017;38:2739-2791.
3. Cruz-Gonzalez I, Sanchez-Ledesma M, Sanchez PL, et al. Predicting success and long-term outcomes of percutaneous mitral valvuloplasty: a multifactorial score. Am J Med. 2009;122:581.e11-e19.
4. Bouleti C, Iung B, Laouénan C, et al. Late results of percutaneous mitral commissurotomy up to 20 years: development and validation of a risk score predicting late functional results from a series of 912 patients. Circulation. 2012;125:2119-2127.
5. Tomai F, Gaspardone A, Versaci F, et al. Twenty year follow-up after successful percutaneous balloon mitral valvuloplasty in a large contemporary series of patients with mitral stenosis. Int J Cardiol. 2014;177:881-885.
6. Fawzy ME, Shoukri M, Al Buraiki J, et al. Seventeen years’ clinical and echocardiographic follow up of mitral balloon valvuloplasty in 520 patients, and predictors of long-term outcome. J Heart Valve Dis. 2007;16:454-460.
7. Lee S, Kang DH, Kim DH, et al. Late outcome of percutaneous mitral commissurotomy: randomized comparison of Inoue versus double-balloon technique. Am Heart J. 2017;194:1-8.
8. Song JK, Song JM, Kang DH, et al. Restenosis and adverse clinical events after successful percutaneous mitral valvuloplasty: immediate post-procedural mitral valve area as an important prognosticator. Eur Heart J. 2009;30:1254-1262.
9. Nunes MC, Tan TC, Elmariah S, et al. The echo score revisited: impact of incorporating commissural morphology and leaflet displacement to the prediction of outcome for patients undergoing percutaneous mitral valvuloplasty. Circulation. 2014;129:886-895.
10. Bouleti C, Iung B, Himbert D, et al. Reinterventions after percutaneous mitral commissurotomy during long-term follow-up, up to 20 years: the role of repeat percutaneous mitral commissurotomy. Eur Heart J. 2013;34:1923-1930.
11. Bouleti C, Iung B, Himbert D, et al. Long-term efficacy of percutaneous mitral commissurotomy for restenosis after previous mitral commissurotomy. Heart. 2013;99:1336-1341.
12. Kim MJ, Song JK, Song JM, et al. Long-term outcomes of significant mitral regurgitation after percutaneous mitral valvuloplasty. Circulation. 2006;114:2815-2822.
13. Chiang CW, Lo SK, Ko YS, et al. Predictors of systemic embolism in patients with mitral stenosis. A prospective study. Ann Intern Med. 1998;128:885-889.
14. Langerveld J, van Hemel NM, Kelder JC, et al. Long-term follow-up of cardiac rhythm after percutaneous mitral balloon valvotomy. Does atrial fibrillation persist? Europace. 2003;5:47-53.
Alec Vahanian, MD
Cardiology Department
Bichat Hospital, University Paris VII
Paris, France
alec.vahanian@gmail.com
Disclosures: Speaker’s fees from Abbott Vascular and Edwards Lifesciences; consultant to Mitraltech Ltd.
Bernard Iung, MD
Cardiology Department
Bichat Hospital, University Paris VII
Paris, France
Disclosures: Speaker’s fees from Boehringer Ingelheim and Novartis; consultant to Edwards Lifesciences.
Advertisement
Advertisement

